When a child is suddenly diagnosed with cancer, it turns your world upside down in seconds. The panic, the questions, and the need to know what exactly you’re facing – especially when names like neuroblastoma and nephroblastoma come up – can be overwhelming. We see this moment every day, and we’re here to ease that storm so you feel a little less alone.
These two cancers may sound similar, but they behave very differently inside the body. One affects nerves, the other the kidneys – adding confusion around symptoms, treatments, and outcomes for families trying to make the best decisions quickly.
As a parent or caregiver, everything starts with clarity – and that’s where we support you, step by step. At our Mumbai clinic, we bring focused care, thorough guidance, and a steady hand when you need it most.
Overview of Neuroblastoma and Nephroblastoma
Every childhood cancer diagnosis brings shock, but when names like neuroblastoma or nephroblastoma are mentioned, the confusion deepens. These tumours differ in many ways – even though they may appear together in medical discussions.
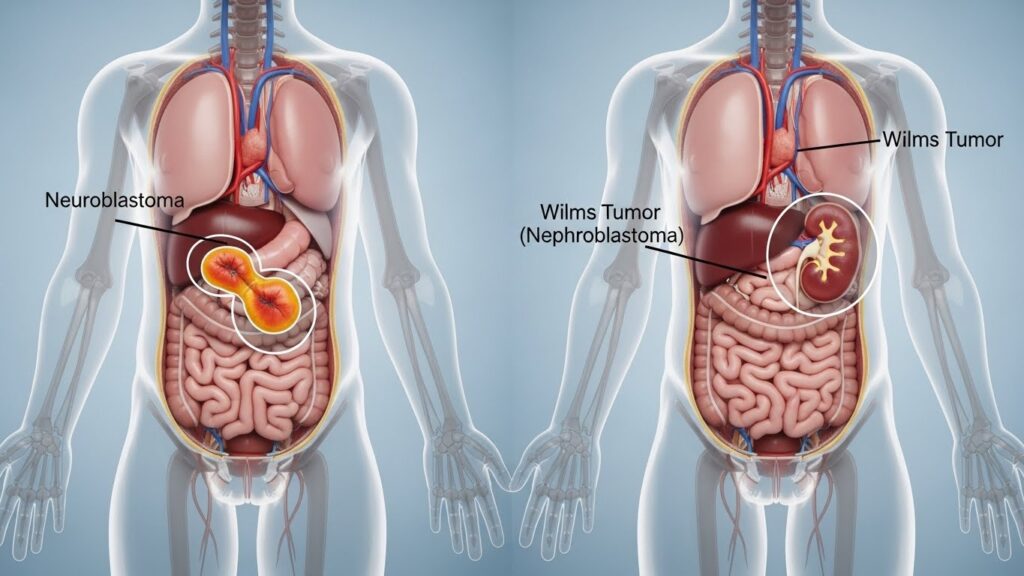
Neuroblastoma grows from nerve tissues, mostly around the adrenal glands, while nephroblastoma begins in the kidneys. At Dr Kriti Hegde’s clinic in Mumbai, we help families learn the differences, so the path ahead becomes a little more certain and your decisions more informed.
General background and prevalence
Neuroblastoma usually strikes earlier, most often in babies under 2 years. Its common site is the adrenal gland, though it can appear near the spine, chest, or belly. It often spreads to the bones, liver, or skin. Nephroblastoma – or Wilms tumour – occurs in slightly older children, mainly between ages 3 to 4. It develops within the kidney itself and usually doesn’t cross over to the other side. It may spread to the lungs or liver but tends to stay more contained.
Tumor biology and origin
Neuroblastoma comes from immature neural cells of the sympathetic nervous system. Some children may inherit the risk through genes like ALK or PHOX2B mutations, and MYCN amplification signals aggressive behaviour. Meanwhile, nephroblastoma arises from immature kidney cells called nephroblasts. This condition may be linked to syndromes like WAGR or Denys-Drash. The WT1 gene often plays a key role, while abnormal kidney development gives rise to this tumour with less aggressive spread than neuroblastoma.
Clinical and Radiological Features
The way each tumour shows up in a child can feel completely different – even if both begin deep inside the abdomen. Symptoms tell an important part of the story, helping specialists like Dr Kriti Hegde decide what to test and what needs immediate care.
Presentation and symptoms
If you notice wide eyes or bruises around a child’s eyes, think of neuroblastoma. That “raccoon eye” sign is linked to metastases in facial bones. It may also bring fever, irritability, and bone pain. If adrenal glands are involved, blood pressure may rise. On the other hand, nephroblastoma presents more quietly – often as a firm, painless lump in the belly. Some children may have mild pain, blood in urine, or constipation. Each has its own subtle warning signs.
Imaging characteristics and diagnosis
Ultrasound helps doctors start the evaluation, but CT or MRI gives more precise views of tumour shape and spread. Neuroblastoma tends to cross body midlines and may appear calcified on scans. MIBG scans pick up neuroblastoma’s active cells and guide further treatment planning. In contrast, nephroblastoma often stays in one kidney, rarely crosses the midline, and seldom shows calcification. It’s best staged using CT scans and surgical findings without a biopsy, unlike neuroblastoma which needs one for confirmation.
Histology, Staging and Risk Stratification
Understanding a tumour at a cellular level changes treatment plans completely. From structure to stage, each clue from the lab or surgery allows more precise care. Dr Hegde and her team rely on these deep insights at every step.
Histopathological features and differentiation
Under a microscope, neuroblastoma shows small, round blue cells that grow in clusters. Some tumours mature and behave less aggressively, while others appear primitive and aggressive. Special stains help confirm the diagnosis, using immunohistochemistry.
Nephroblastomas, meanwhile, show a mixture of blastemal, epithelial, and stromal elements – more structured than neuroblastoma. Better organised tissue usually means a better outlook. Tissue samples help sort tumours into favourable or unfavourable categories, which directly affects survival guesses and treatment plans.
Staging systems
Children with neuroblastoma are staged using INSS (post-surgery-based) or INRGSS (before surgery). There’s even a special “4S” group seen only in very young babies where the tumour may surprisingly shrink on its own. Risk groups guide therapy – from surgery alone to bone marrow transplants. Nephroblastoma staging follows COG or SIOP systems which classify based on how much tumour remains or spreads. Stage V means both kidneys are affected. These systems serve as roadmaps for future care.
Treatment Approaches
Once the diagnosis and stage are clear, treatment starts – sometimes within days. The tools are similar – surgery, chemo, radiation – but how and when they’re used differ greatly for each cancer. Having expert direction keeps the plan steady.
Therapy protocols and surgical approaches
In neuroblastoma, timing is everything. Some children need immediate chemotherapy based on risk level. Drugs like carboplatin or etoposide tackle the tumour before surgery becomes safer. If surgery is possible early, full removal helps.
Afterward, radiation and even stem cell transplants may follow. Nephroblastoma usually begins with surgery – removal of the kidney is the first line when the tumour hasn’t spread. Chemotherapy often follows using vincristine or doxorubicin to ensure full control. Radiation is reserved for stubborn or late-stage disease.
Targeted therapies and future directions
Newer therapies bring added hope. In high-risk neuroblastoma, immunotherapy targets tumour cells with precision, while MYCN-targeted approaches push survival higher. MIBG therapy delivers radiation inside the tumour cells directly.
For nephroblastoma, future approaches are evolving through ongoing trials. Though not as common as in neuroblastoma, certain molecular therapies are being tested. Dr Hegde engages with the latest research and offers qualified children access to trials, shaping treatments with science as it grows.
Key Differences Between Neuroblastoma and Nephroblastoma
Clear information brings peace of mind. When comparing these two cancers, side-by-side contrasts help families and doctors make faster, better-informed choices.
Summary comparison chart
✔ Age at onset: Neuroblastoma – mostly before 2 years; Nephroblastoma – 3 to 5 years
✔ Tumour location: Neuroblastoma – adrenal glands/sympathetic chain; Nephroblastoma – kidney
✔ Spread: Neuroblastoma – bone, skin, liver; Nephroblastoma – mainly lungs
✔ Diagnosis tools: Neuroblastoma – biopsy, MIBG, catecholamines; Nephroblastoma – imaging, resection
✔ Staging and risk: Neuroblastoma – INSS/INRGSS; Nephroblastoma – COG/SIOP
✔ Treatment: Neuroblastoma – chemotherapy, surgery, immunotherapy; Nephroblastoma – surgery first, then chemo
Clinical relevance in diagnosis and management
Misdiagnosis between these two tumours can set back treatment. Imaging helps, but close collaboration between oncologists, radiologists, and pathologists ensures the best clarity.
Families benefit from Dr Kriti Hegde’s multidisciplinary team in Mumbai, where all specialties work under one roof.
This model shortens delays, anticipates complications, and adjusts treatment with precision. Early detection improves survival, but correct diagnosis defines everything. When these efforts come together, care shifts from guesswork to guided, confident decisions.
FAQs
Does the tumour cross the midline?
Yes, neuroblastoma often crosses the midline due to its spread from the nerve chain. Nephroblastoma usually remains confined to one kidney.
Presence of calcifications: what does it imply?
Calcifications are more common in neuroblastoma and usually absent in nephroblastoma, making it a helpful clue in scans.
What is the rule of 10 in nephroblastoma?
It’s not commonly used in nephroblastoma like in other tumours such as pheochromocytoma. However, 10% of Wilms cases do show up in both kidneys.
How to distinguish from other small round blue cell tumours?
Other tumours like lymphoma or rhabdomyosarcoma may look similar under the microscope. Immunohistochemistry and genetic testing help in clear diagnosis.
What is the role of biopsy in uncertain cases?
For neuroblastoma, a biopsy is crucial for diagnosis. For Wilms tumour, surgery often comes first to avoid tumour spilling and spreading.
What if the tumour is non-MIBG avid?
In such cases of neuroblastoma, PET-CT scans can help. Tumours may still be identified through FDG uptake, helping to track treatment effectively.
Worry Has a Way of Knocking the Wind Out of You
When your child is unwell and every test brings more questions than answers, peace becomes a distant memory. Clarity, especially between two diagnoses that sound confusingly similar, can make all the difference in how you sleep at night and how you move forward with treatment.
The best next step is understanding what sets these two conditions apart, so you can act with confidence. This knowledge offers direction, lends comfort, and helps you plan ahead without hesitation sitting in the driver’s seat of uncertainty.
At our clinic led by Dr Kriti Hegde in Mumbai, we help families face crucial moments like these with expert support and transparent care. Book a consultation so we can walk this path with you, fully prepared and never alone.